Colloidal silver is a popular supplement used for a spectrum of perceived health benefits. However, the FDA does not regulate it and, in fact, issued a final rule deeming it “not generally recognized as safe and effective.”
Arising from excessive silver exposure, argyria is a rare condition characterized by a slate-blue discoloration of the skin and mucous membranes. This report highlights a specific dermatologic finding seen in chronic silver poisoning and discusses occupational, environmental, and pharmacologic risk factors.
Recognizing chronic argyria is important to the emergency physician in forming a targeted differential for the “blue patient” and avoiding unnecessary workups or medications that may harm the patient.
Case Presentation
A 79-year-old female with a history of chronic kidney disease stage V and chronic argyria presented to the ED with subclinical fever, fatigue, and mild joint pain. She had been experiencing these symptoms for 6 weeks and had multiple unremarkable laboratory work-ups in the ED. Incidentally, on physical examination she had deep bluish pigmentation of the face, conjunctiva, tongue, and upper extremities, which she stated is her baseline from her chronic argyria.

Image 1. Skin color changes are a hallmark of chronic argyria
This patient’s chronic argyria resulted from use of homeopathic silver-containing oral supplements she had been using to treat chronic sinus congestion for 8 years. She denied any chest pain, shortness of breath, or new skin discoloration. Her workup demonstrated a non-specific leukocytosis of 13.8 thousand/mcL, and a mild anemia of 10.4gm/dL with a mean corpuscular volume of 103 fL. She also had a creatinine of 3.72mg/dL with a GFR of 12mL/min, both of which consistent with her baseline kidney disease. Urinalysis and remaining serology were unremarkable.
Given the presence of non-specific symptoms and multiple prior ED visits without a definitive answer, CT imaging with contrast of the neck, chest, abdomen, and pelvis was obtained to evaluate for neoplastic lesions and presence of lymphadenopathy. There was no evidence of lymphadenopathy; however, a pathological T6 vertebral compression fracture with sclerotic lesions was noted. The patient was ultimately discharged with instructions to pursue outpatient follow-up for the sclerotic lesions and compression fracture.
Case Discussion
Argyria is a rare but important differential diagnosis, especially in emergency medicine, due to its distinctive appearance. Argyria is a characteristic dermatologic finding seen in chronic silver toxicity. The blue-gray discoloration can result from mechanical contact of silver particles on the skin or via inhalation or ingestion of silver particles. Silver particles that are systemically absorbed dissolve into silver ions, which can be reduced by sunlight or sulfur and lead to increased melanin production in light-exposed areas and blue discoloration when alongside selenium ions.1
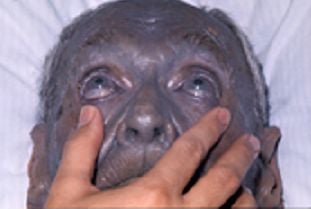
Image 2. Generalized argyria stemming from nose drops containing colloidal silver, resulting in permanent pigmentary changes. (credit Herbert L. Fred, MD and Hendrik A. van Dijk)
Chronic argyria is suspected to signal worsening kidney function, based on limited data.2 While the link to long-term silver therapy and renal failure has not been definitely linked, effects of such therapy on the kidney should be considered when managing patients with argyria, especially when considering the administration of nephrotoxins. In addition to this, there are significant impacts to the cardiac, hepatic, and hematopoietic systems seem from silver toxicity, with manifestations such as ventricular hypertrophy, bone marrow suppression, hepatic necrosis, vertigo, seizures, and acute tubular necrosis.1
Chronic exposure to silver and the subsequent accumulation of these deposits are often due to either occupational exposure or use of silver-containing supplements. A higher degree of suspicion for generalized argyria should be held in those with long-term occupations involving the manufacturing of silver-containing products, including antiseptic agents, porcelain, dyes, and jewelry.3 Others develop systemic argyria secondary to unregulated homeopathic supplements, as is the case for our patient, as well as buying colloidal silver, photography products, mirrors, plating, inks and dyes, and porcelain over the counter. Treatment of chronic argyria is difficult because it is irreversible and not amenable to chelation; however, there may be some benefit from topical hydroquinone 5% and laser technology.
Treating the “Blue Patient:” What Else Could it Be?
Apart from argyria, the differential for the “blue patient” is broad yet important for the ED physician to consider. Methemoglobinemia, a disorder of hemoglobin during which ferrous (Fe2+) iron in hemoglobin is oxidized to the ferric (Fe3+) state, is classically attributed to toxicity from local anesthetics, nitrates, dapsone, phenazopyridine, quinones, sulfonamides and other pharmaceuticals; however can also be seen in patients with sequelae of severe fire injuries, as well as those with hereditary conditions such as NADH methemoglobin reductase deficiency.4 High-flow oxygen and methylene blue are the mainstays of treatment. It should be noted that large doses of methylene blue, typically greater than 7 mg/kg, have been reported to rarely cause initial blue skin discoloration and paradoxical methemoglobinemia.3
Blue skin pigmentation from chrysiasis may be seen in patients who have undergone prolonged parenteral gold therapy.5 In cases of skin discoloration secondary to long-term amiodarone toxicity, medication review and addressing cardiac concerns are vital as blue pigmentation from amiodarone use has been shown to be reversible.6 Overall, the ED plays a crucial role in diagnosis, initiation of appropriate treatments, and ensuring patient safety and comfort.
EM TAKEAWAYS
- Chronic argyria, characterized by severe blue skin discoloration due to excessive silver exposure, is a rare but noteworthy condition for emergency physicians to consider in the “blue patient.”
- This case underscores the importance of a thorough evaluation and differential diagnosis in the ED, given the broad differential of dramatic blue skin discoloration.
- Long-term silver therapy can affect multiple systems, including cardiac, hepatic, hematologic, and kidneys, warranting careful consideration in patient management.
References
- Lai-Becker M, Burns M. Silver. In: Goldfrank’s Toxicologic Emergencies. McGraw Hill Education; 2019:1344-1347.
- Rosenman KD, Seixas N, Jacobs I. Potential nephrotoxic effects of exposure to silver. Br J Ind Med. 1987;44(4):267-272.
- Mackison FW. NIOSH/OSHA—Occupational Health Guidelines for Chemical Hazards. Washington, DC: US Government Printing Office; 1981.
- Price D. Methemoglobin Inducers. In: Goldfrank’s Toxicologic Emergencies. McGraw Hill Education; 2019:1703-1712.
- Cohen PR, Ross EV. Q-Switched Alexandrite Laser-induced Chrysiasis. J Clin Aesthet Dermatol. 2015;8(9):48-53.
- Jolly U, Klein G. Blue man syndrome. CMAJ. 2016;188(8):604.



